Glaucoma is a disease affecting an estimated 60.5 million people worldwide and 5.7 million people in the United States. Globally, it accounts for 8% of all cases of blindness and is the leading cause of irreversible blindness worldwide. In the United States, it accounts for an approximate annual cost of $1.5 billion. Initial therapy for glaucoma typically consists of topical eye drops or laser trabeculoplasty, both of which aim to lower intraocular pressure and have similar efficacy. Historically though, when pharmacologic and/or laser treatment fails to control IOP, incisional surgery is required. Despite their efficacy, these surgical interventions have greater risks, require frequent follow-up and prolonged recovery time. Therefore, these procedures are often delayed in mild to moderate disease and reserved for patients with more severe disease who warrant aggressive intervention. However, in the last two decades the field of glaucoma has seen the advent of micro invasive glaucoma surgery (MIGS) which has sought to fulfill the unmet need for improved treatment options and close this treatment gap.
Patients generally are good candidates for MIGS if they have mild to moderate glaucoma, are intolerant or noncompliant with drops, or if their IOP is not controlled with topical eye drops or laser trabeculoplasty. MIGS procedures can also be used to reduce drop dependence at the time of cataract surgery in patients whose disease may be well controlled. MIGS can be done in combined together for maximum effect.
iStent
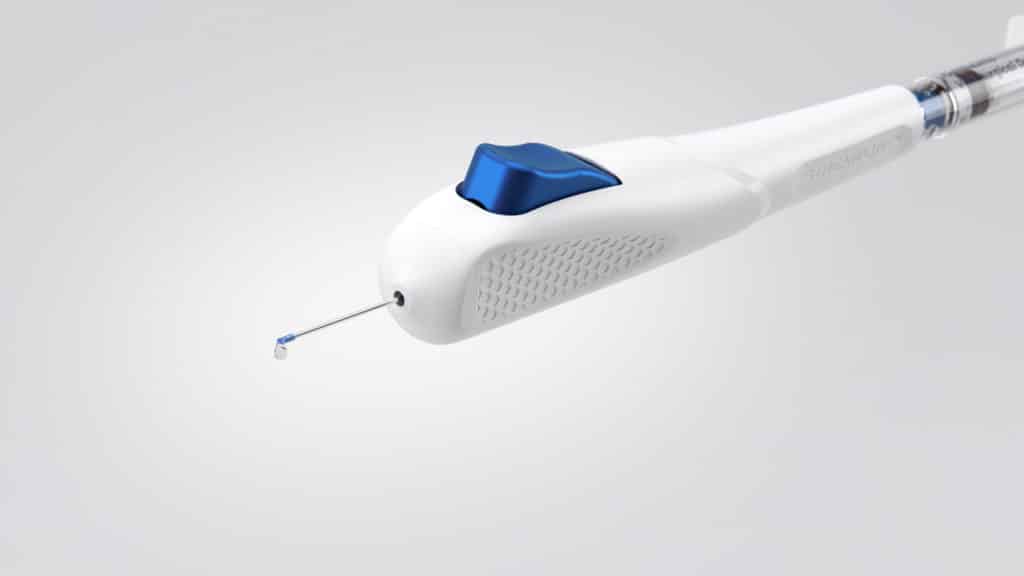
The iStent Inject is the second generation trabecular meshwork bypass stent which received FDA approval in June 2018. The iStent inject is the smallest device to be implanted in the human body and, like the first generation iStent, is composed of heparin-coated, non-ferromagnetic titanium. The iStent inject consists of a single-use injector that comes pre-loaded with two devices, which are to be placed 2-3 clock hours apart in the nasal angle at the time of cataract surgery.

Streamline Canaloplasty
This procedure aims to improve the conventional outflow fluid pathway to reduce pressure in the eye. This can be done at the time of cataract surgery or as a standalone procedure and is very effective in treating glaucoma.